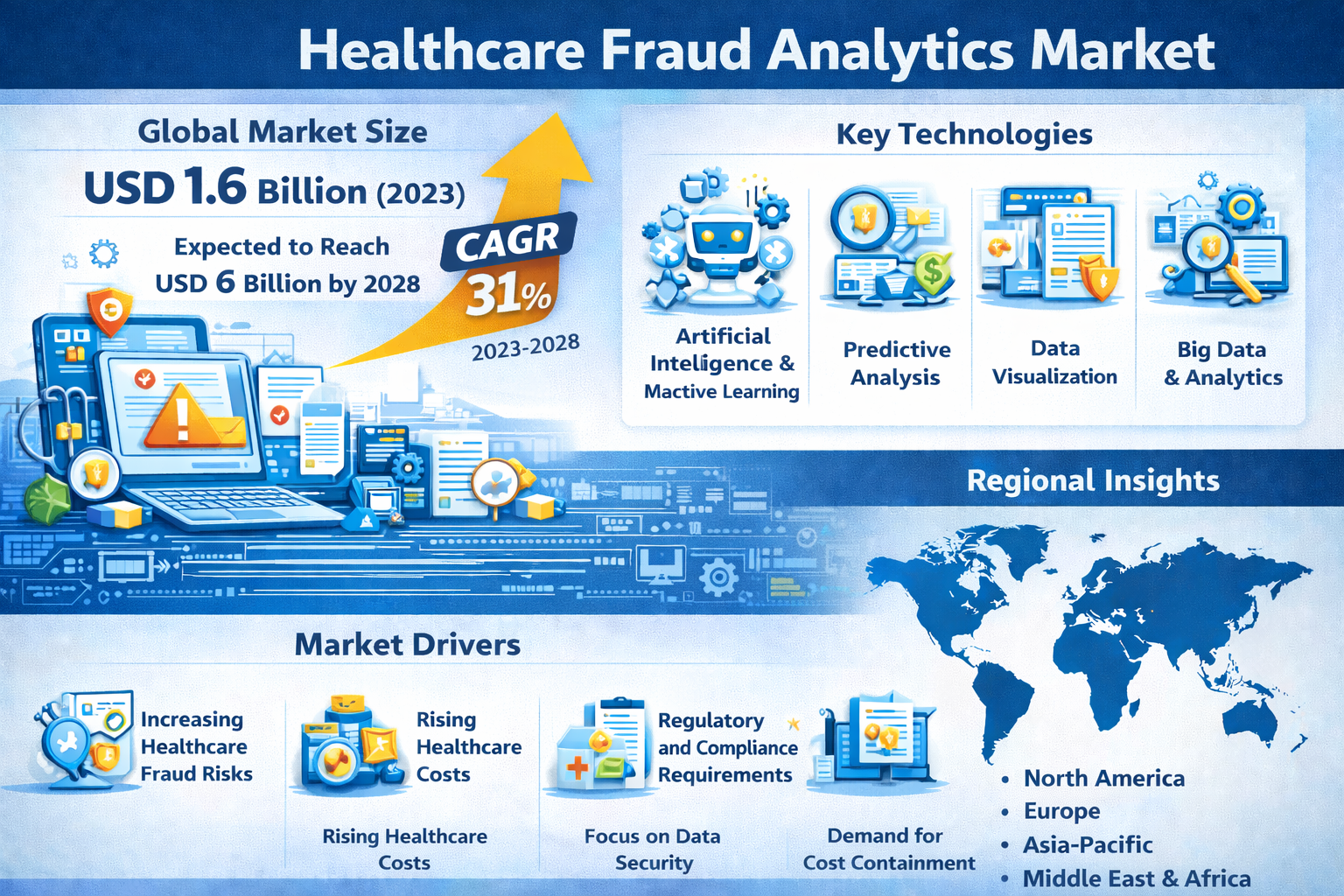
The global Healthcare Fraud Analytics Market Growth is witnessing strong expansion, fueled by rising fraud incidents, increasing healthcare expenditure, and the rapid adoption of advanced analytics technologies. According to The Insight Partners, the market is projected to reach approximately US$ 61.01 billion by 2031, growing at a CAGR of 11.0% during 2025–2031.
The growing complexity of healthcare billing systems, combined with the surge in insurance claims and digital healthcare transactions, is accelerating demand for fraud detection and analytics solutions. Healthcare providers, insurers, and government agencies are increasingly deploying advanced tools to improve transparency, reduce losses, and enhance operational efficiency.
Get Sample PDF @ https://www.theinsightpartners.com/sample/TIPRE00008954
Market Trends
Rapid Integration of Artificial Intelligence and Machine Learning
One of the most prominent trends shaping the Healthcare Fraud Analytics Market is the integration of artificial intelligence (AI) and machine learning (ML). These technologies enable automated fraud detection, real-time anomaly identification, and predictive risk assessment. AI-driven systems are transforming traditional rule-based models into intelligent platforms capable of detecting complex fraud patterns with higher accuracy.
Shift Toward Real-Time Fraud Detection
Healthcare organizations are increasingly adopting real-time analytics solutions to detect fraud before claims are processed. Real-time monitoring allows insurers and providers to identify suspicious activities instantly, reducing financial losses and improving operational efficiency. Advanced streaming technologies are further enhancing the ability to process large volumes of data in milliseconds.
Growing Adoption of Cloud-Based Solutions
Cloud-based healthcare fraud analytics platforms are gaining significant traction due to their scalability, flexibility, and cost-effectiveness. These solutions enable organizations to process large datasets efficiently and support remote access, making them ideal for modern healthcare ecosystems. The shift toward cloud deployment is expected to accelerate market growth during the forecast period.
Emergence of Blockchain for Transparency
Blockchain technology is emerging as a key trend in healthcare fraud analytics. It enhances transparency and security in healthcare transactions by creating immutable records. This technology helps reduce data manipulation and ensures accurate tracking of medical billing and claims processes, contributing to improved fraud prevention.
Increasing Focus on Patient-Centric Fraud Prevention
Healthcare organizations are adopting patient-centric approaches to fraud prevention, focusing on improving transparency in billing and enhancing trust. By providing clear insights into medical charges and claims, analytics solutions help reduce disputes and improve patient satisfaction.
Market Growth Analysis
Rising Incidence of Healthcare Fraud
The increasing number of fraudulent activities, including false claims, billing manipulation, and identity theft, is a major factor driving market growth. As fraud schemes become more sophisticated, the demand for advanced analytics solutions continues to rise, encouraging healthcare organizations to invest in robust fraud detection systems.
Expansion of Health Insurance Coverage
The growing penetration of health insurance globally is contributing to the increasing volume of claims, which in turn raises the risk of fraud. This trend is driving the adoption of healthcare fraud analytics solutions among insurance providers to ensure accurate claim processing and minimize financial losses.
Digital Transformation of Healthcare Systems
The rapid digitalization of healthcare, including the adoption of electronic health records (EHRs), telemedicine, and mobile health applications, is generating vast amounts of data. While this improves efficiency, it also increases vulnerability to fraud. Analytics solutions play a critical role in monitoring digital transactions and identifying irregularities, thereby supporting market growth.
Growing Demand for Predictive and Prescriptive Analytics
Predictive and prescriptive analytics are gaining prominence as organizations shift from reactive to proactive fraud detection strategies. Predictive models analyze historical data to identify potential risks, while prescriptive analytics provide actionable insights to prevent fraud. These capabilities are significantly enhancing the effectiveness of fraud management systems.
Regulatory Pressure and Compliance Requirements
Governments and regulatory bodies worldwide are implementing stringent policies to combat healthcare fraud. Compliance requirements are pushing organizations to adopt advanced analytics solutions that ensure transparency, maintain audit trails, and support regulatory reporting. This regulatory push is a key growth driver for the market.
Increasing Investments in Healthcare IT
Rising investments in healthcare IT infrastructure are further fueling market growth. Organizations are allocating significant resources to adopt advanced analytics platforms, integrate AI technologies, and enhance data security, creating a strong foundation for the expansion of healthcare fraud analytics solutions.
Competitive Landscape and Key Players
The Healthcare Fraud Analytics Market is highly competitive, with leading players focusing on technological innovation and strategic partnerships. Key companies operating in the market include:
- SAS Institute Inc.
- IBM Corporation
- Wipro Limited
- HCL Technologies
- Relx Group PLC (LexisNexis Risk Solutions)
- Northrop Grumman
- OSP Labs
- Scio Health Analytics
- CGI Group Inc.
These companies are investing in AI-driven analytics, cloud-based solutions, and real-time data processing capabilities to strengthen their market presence and address evolving customer needs.
Conclusion
The Healthcare Fraud Analytics Market is poised for substantial growth by 2031, driven by key trends such as AI integration, real-time analytics adoption, and cloud-based deployment. Increasing fraud incidents, expanding health insurance coverage, and rapid digitalization are further accelerating market expansion.
With a projected CAGR of 11.0%, the market offers significant opportunities for technology providers and healthcare organizations. As fraud detection becomes more sophisticated, advanced analytics solutions will play a crucial role in ensuring transparency, reducing financial losses, and enhancing the overall efficiency of healthcare systems worldwide.
Related Reports
1 Healthcare Fraud Detection Market
About Us:
The Insight Partners is among the leading market research and consulting firms in the world. We take pride in delivering exclusive reports along with sophisticated strategic and tactical insights into the industry. Reports are generated through a combination of primary and secondary research, solely aimed at giving our clientele a knowledge-based insight into the market and domain. This is done to assist clients in making wiser business decisions. A holistic perspective in every study undertaken form an integral part of our research methodology and makes the report unique and reliable.
Contact Us: If you have any queries about this report or if you would like further information, please contact us:
The Insight Partners
E-mail: sales@theinsightpartners.com
Phone: +1-646-491-9876
Website: www.theinsightpartners.com